How is PAH diagnosed?
Pulmonary arterial hypertension (PAH) is rare and can be difficult to diagnose. Many people live with symptoms for years before learning they have PAH. If your doctor thinks you may have PAH based on your symptoms, you may need several tests to confirm or rule out a diagnosis of PAH.
A right heart catheterization (sometimes shortened to “right heart cath” or “RHC”) is the test doctors use to confirm PAH. Your care team may order other tests first to look at the cause of your symptoms, but only the right heart cath can clearly determine if you have PAH.
The role of testing in PAH
Testing is an important part of PAH care. After tests help show if your symptoms may be caused by PAH and confirm a diagnosis, they help you and your care team follow your progress and see how your PAH may change over time. They also help guide your treatment plan.

“When I was diagnosed I had no idea what PAH was; I had never heard of it. I was in shock and felt like, ‘How am I going to live with this disease?’ … But I also started feeling so much better after my body got used to the medications.” —Nancy, PAH Initiative Patient Ambassador
Types of PAH tests
From diagnosis to risk assessment
Testing often begins with a physical exam and a review of your medical and family history, since PAH can sometimes run in families. Some of the same tests that help confirm PAH are repeated later to monitor your risk status—showing how you are doing today, how you may feel better with adding or adjusting treatment, and how well you may do in the future.
Tests focused on your right heart and lungs
Pulmonary function tests (PFTs) measure how well your lungs are working:
- How much air moves through your lungs—and how much air your lungs can hold
- How quickly air is pushed through your lungs
Echocardiograms (Echos) often raise doctors’ concern for PAH before a right heart cath confirms the diagnosis. Echos remain vital as a noninvasive way to monitor changes in the heart that reflect disease progression or improvement. Using soundwaves, Echos can help your specialist:
- Measure blood flow through the heart and any changes in its size and shape
- Evaluate how well your heart’s right side is working
Right heart catheterization measures the pressures in the right side of your heart and the lungs. High pressures are a sign of narrowed vessels in the lungs. A right heart cath:
- Usually happens after a full diagnostic evaluation
- May also be used for monitoring and tracking changes over time
Learn more about what to expect from a right heart cath, including why it’s ordered and the important information it provides
Right Heart CathNT-proBNP and BNP blood tests are simple, informative blood tests that show how hard your heart is working and how much strain it’s under:
- Before PAH diagnosis, blood tests can signal the need for further testing (like Echo) to identify causes of heart strain
- After PAH diagnosis, blood tests are used to monitor your PAH and how well your treatment plan is working
Tests focused on your ability to exercise and do daily activities
6-minute walk test measures your ability to exercise by measuring the distance you can walk in 6 minutes.
- May also be used for monitoring by comparing your results over time
- Walking longer distances can be a sign that your PAH is improving
How far you can walk reflects how well your heart and lungs are working together
Functional Class captures how PAH affects you day to day. Functional Class:
- Is evaluated during a clinical assessment
- Classifies how severe your symptoms are during everyday activities
Learn more about the 4 Functional Classes and how your doctor determines yours
Functional ClassOther tests (if needed based on your circumstances)
- Genetic testing for unexplained (idiopathic) PAH, family history of PAH, or PAH linked to congenital heart disease
- Blood tests to check kidney and liver function, electrolytes, blood counts, HIV status, and antibodies for connective tissue disease (CTD)
- Ventilation/Perfusion (V/Q) scan to check for blood clots in the lungs (linked to a different type of PH)
- Sleep study for patients with possible sleep apnea (also linked to a different type of PH)
- Other imaging tests like chest CT or liver ultrasound, if recommended by your care team
Your tests, explained
Watch PAH expert Dr. Lana Melendres-Groves explain the science behind PAH symptoms, how to get ahead of future symptoms, and what to discuss with your doctor if yours are not improving.
Welcome to the PAH Today National Broadcast Series. My name is Dr. Lana Malenda-Groves, and I’m the medical director for the Pulmonary Hypertension Program at the University of New Mexico. It is my pleasure to join you today to discuss the tests that you get when you’re being evaluated for your PAH.
First, let me give this disclaimer: This presentation is sponsored by and made on behalf of United Therapeutics. Speakers are compensated by UT. The information presented here is for educational purposes to aid the patient-doctor relationship and is not intended for professional medical advice. Always discuss your individual test results and any questions you may have with your health care provider.
All right, so we sort of have a full agenda today. To give an overview of what this is all about: tests. Often, like when we were back in school, tests seem scary. We get nervous for them; we try to prepare for them. But at the end of the day, the hope with this presentation is to talk you through each step of the way so that when you know a test is coming up, you will feel prepared.
So first, we’re going to talk about why testing is so important, next what those test results may actually mean, and then how we combine those test results to give us even further information, and last, what you can do.
So first, why testing is so important. As I mentioned before, when we think about testing, it takes us back to our childhood and having to go into school, being prepared to take a test that you feel like, “What if I don’t do well?” That isn’t the goal of these tests. Just like in school or when you took your driver’s test, the goal is to gain an understanding of where your strengths may be and where your weaknesses may be. That way, you can work on those weaknesses and continue to build on those strengths.
When testing in PAH, we also are trying to understand what the body is telling us: maybe what its strengths are in that moment as well as what its weaknesses are. So by doing regular testing when it comes to PAH, it helps to inform your provider, as well as yourself, about decisions that may need to be made for your care. That starts at the very beginning with the screening and evaluating the likelihood that somebody may have PAH as a diagnosis, but it doesn’t stop there. As somebody is diagnosed with PAH, we then have to be able to assess how they’re doing along their journey. That usually comes along with treatments and treatment plans, and by getting testing, we’re able to evaluate what those therapies or treatments may have done. Then we’re able to further monitor and sort of track the disease status. So all of these results may indicate that an adjustment may be made for your treatment plan.
I really like thinking of PAH as a puzzle, because like many of us, throughout our life, we’ve done puzzles together, and I can tell you how tremendously frustrating it is when you’ve worked so hard, you’ve gotten to the end of your puzzle, and you’re missing a piece or two. You look on the floor, and you try to find it everywhere, and no matter what you do, all that hard work, all that beauty in front of you, is hard to be able to put fully together because you may be missing a piece or two. It’s the same in PAH. We think about it in terms of all of these single tests that we do, but it’s really putting all those tests together to create this overall image of what that individual is going through that helps us to understand what they may need. But in order to understand why the different tests are important and neat and necessary, it’s really important to once again review how PAH affects the body.
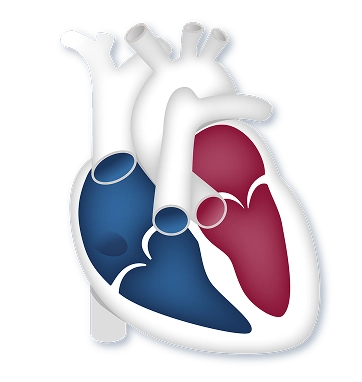
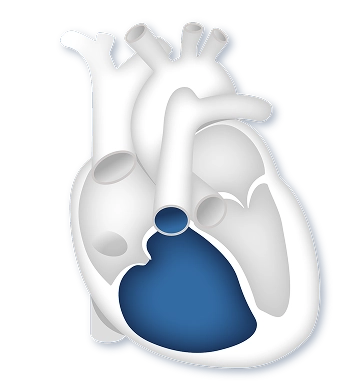
Now, whether you’re new to this PH journey, or your loved one is just beginning their journey, or maybe you’ve been doing this for many, many years and have a very good sense of how your body feels and what it’s going through, I think it’s always important to really look back and have an overview of PAH and how it affects the heart, lungs, and blood vessels in the lungs. So to start off, in PAH, the walls of the blood vessels in the lungs begin to thicken and narrow. As those vessels narrow, it causes the resistance to blood moving through those blood vessels, or the blood flow, to become more difficult. That resistance goes up. As that resistance goes up in the blood vessels, the heart has to work harder in order to pump blood through the lungs, and as the right heart starts to work harder to pump that blood through the lungs, it starts to enlarge or grow larger and more muscular, and it becomes more and more difficult for it to continue working so hard and pumping that blood through the lungs. Over time, we can see that the heart becomes strained from that extra work and is unable to keep up with the extra workload that it’s being asked to perform.
We often are able to see the results of the heart not keeping up based off of some of someone’s symptoms. Frequently, someone may describe feelings of shortness of breath or difficulty breathing, not being able to catch their breath, or they may start to sense an irregular or kind of abnormal sensation or heartbeat. They may have chest discomfort or chest pain, or they may sense that their abdomen has gotten more swollen, or that their legs seem to be retaining fluid. All of those things are indicators that the right heart may be struggling. So these tests that a PAH specialist is asking for can help to give information about how the heart and the lungs are doing, and sometimes it can even give that information before someone is even feeling those symptoms.
So, what do these tests actually mean? Well, I think that most of you have gone to a physician or a provider at some point, and they put you on a scale or they took your blood pressure, and they always record that. Then the next time you go in, they compare that to what those results were the last time. It’s very similar in terms of the testing that we get in PAH. The specialists are comparing test results over time. Usually, it’s comparing them to your own test results to better understand how you individually are doing. But we also have thousands and thousands of records and information that have given us certain thresholds, or what we call benchmarks, that we’re working to get our patients beyond. And so we then utilize the tests and the results we get for one person to then compare that to a large number of people, which gives us a sense of how someone may do long term.
Now, there are different types of tests that we get for PAH. Some of them are very much focused on the right side of the heart and how the lungs are doing, and other tests are more looking at how somebody’s doing in terms of their ability to exercise or do their daily activities. So we’re going to talk about both of those things, but we’re going to start with four key tests that focus on the right side of the heart and the lungs. Some of you may have had all of these tests; some of you have may not have gone through any of these tests yet and may just be in the midst of getting worked up.
The first test that we want to talk about are going to be pulmonary function tests, or lung tests. Then we’ll talk about the right heart catheterization, a blood test called an “NT-proBNP” or a “BNP,” as well as talking about the echocardiogram.
Now, when it comes to pulmonary function tests, these are really tests that are just looking at how well do your lungs work. We measure them in different ways, and often when I ask my patients about, “Have you ever had pulmonary function tests?” that doesn’t mean a lot. When I say, “Did they put you in a little tube where then they told you to breathe, breathe, breathe, go, go, go? You have a respiratory therapist cheering you on,” then they remember, “Oh, yes, I have had those,” or clearly they haven’t. Really what these tests are looking at are: how much air can your lungs hold, how does that air move through your lungs, and how quickly are you able to push that air out from your lungs? This information helps us to understand if potentially the blood vessels are maybe not functioning as well as we would like them to. It also gives us a tremendous amount of information just about how the lungs function. Frequently, we’re getting these tests at the beginning of someone’s journey during their diagnosis period, but often we repeat these tests throughout time to understand if they’re changing.
Now I’d like to talk about right heart catheterizations. Many of you may have already undergone a right heart catheterization, and as you may or may not know, it is used to measure the pressures in the heart and the blood vessels in the lungs. There is a very low risk in undergoing a right heart catheterization, and I know at times invasive tests can feel scary, but it is extremely important to be able to definitively diagnose PAH through a right heart catheterization. What we measure are the pressures inside the right side of the heart, and with the catheter, are able to measure the pressure in the blood vessels as well as to calculate the resistance in those blood vessels. This gives us a tremendous amount of information as to what may need be needed in your care, as well as later on, we may use it to monitor your disease and repeat that procedure to be able to compare to where you started.
All right, now we’ll move on to a blood test. This is something I frequently get on my patients because although nobody likes getting their blood drawn, it is a very simple way to gain a lot of information. The NT-proBNP and BNP can reveal how hard your heart is working, or if it is struggling. The level of these in someone’s blood will indicate if, for instance, their heart seems to be functioning and working normally, or if maybe the heart is under more strain than we would like it to be. And so these help us to understand if we should be changing therapies or treatments for our patients.
Now moving on to the echocardiogram, or as many of you may know it as, is an Echo. This tells your health care provider about changes in your heart. We use non-invasive sound waves to be able to gain information that gives us a visual picture of what the heart looks like. That may be able to indicate if there are changes in the size and shape of the heart, how that blood flow is moving from chamber to chamber and then into the lungs. It can also evaluate realistically an overall function of the right side of the heart. Now we frequently use this when we change therapies or when somebody’s returning to see us, but it is often used for simply monitoring your disease over time. Again, it’s those pieces of the puzzle as we move forward in your journey to be able to compare, and that may indicate whether a treatment plan change is required.
These changes in the heart frequently occur before anyone ever has symptoms, and that’s always a concern not only for patients but for us as providers, because frequently if we’re waiting for somebody to come in and tell us that they feel differently, we may have missed opportunities to really impact how somebody does long term. So frequently those changes occur in the heart, and then after that we often see that the blood tests may change. Those blood tests may increase, indicating that the heart’s under more strain, and yet someone physically and symptomatically may not have felt anything yet. Then we start to see changes in someone’s exercise or their Functional Class, their ability to do their activities, and we can often see this as well on what we call our six-minute walk distance, looking at how far someone might be able to walk in that period of time. All of these things seem to occur before anybody would end up hospitalized, which we hope to not happen for any of our patients. And so that’s why we go back to trying to get tests before somebody actually becomes more symptomatic in order to try and make changes and improve them long term.
So, as I mentioned, these tests sometimes focus on the heart and lungs, and the importance of that is understanding how those lungs work and the impact on how those lungs may be affecting the heart’s ability to function. We’re able to assess the size, the shape, and the function of the right side of the heart, which provides us information on whether the heart may be under strain. The Echos are generally something that we do more often because they’re non-invasive, and they can give us really good valuable information that helps us in our response and what we may suggest or recommend for our patients’ treatment.
Now, moving more into how you’re doing, these are tests that really are focused on the individual and their ability to do their daily activities and their exercise. We call them Functional Class and six-minute walk tests. Now the Functional Class, it’s interesting because it really is something to try to just gain a better understanding of what each person does every day. Obviously, everybody is different, and this is why it’s so essential that the lines of communication are open between a patient and their provider or their physician. Because having that discussion and understanding what my patient is able to do today, in comparison to what they used to be able to do, and what we would like them to be able to do, really helps to capture their picture of Functional Class.
We talk about a class one, and the bicycle’s there, but it doesn’t mean you need to go be riding a bike or running. It really means that you can do anything that you need or want to do without feeling those symptoms. That Functional Class two is that you can do all of your normal activities, but when you start to do something just a little bit extra, putting a little extra strain on the body, that you may feel some of those symptoms of shortness of breath or fatigue. When we get into a class three and class four, that really is an indication that our patients are much more symptomatic on their daily basis, doing things like making the bed or trying to clean themselves up or clean up their home, and that they start to feel those symptoms, and that impedes their ability to do the things that they would like to do. And by the time someone is to that Functional Class four, they really are feeling symptoms when they’re just resting. So we really would like to be able to get all of our patients to a place that they can do the activities that they want to do throughout the day without limitation.
One of the ways that we may measure this in our offices would be to do a six-minute walk test. This tracks somebody’s ability to sort of do exercise over time. Now it doesn’t necessarily reflect what you do every day, because I’m not sure a lot of us go out and time ourselves for six minutes to do a walk. But on the other hand, by having that information, it is something that’s very easily reproducible, and we can then measure it over time. We’re able to see if there’s consistency with those tests in that either your test looks exactly as it did the prior time that you were there, and maybe that’s exactly where we’d like you to be, or maybe you’ve gained in how far you can walk on your current test, which is a reflection of potentially what we’ve changed in your treatment plan. Or maybe we’re on the other side of that spectrum where you used to be able to walk further, and now we’re starting to see a drop off in that, which would be an indication to consider what might need to be done to get you back to where you had been.
Now we’ve had an opportunity to talk about different types of tests. Previously, we talked about the tests that really look at how the heart and lung are working, and now we’ve talked about the testing that really looks at the ability to exercise and do activities. I think that it’s important to distinguish between the two types of tests. One really helps us potentially understand what may be happening before somebody feels symptoms, and some of the tests, when we’re really looking at your ability to exercise and do activities, may often be something that now the changes have occurred in the heart and lungs, and you’re feeling them. So we really do like to be able to combine these types of tests to be able to understand and move on information to never allow you to get worse in terms of your disease state, and instead, only continue to look to betterment and improvement. So it’s important to remember to talk to your providers about any symptoms that you may have or are changing, but it is also important that we as providers are always thinking and anticipating in advance of what may be occurring to you from a symptom standpoint.
All right, so now we’re coming to taking those pieces and starting to build our puzzle. We’ve flipped them all over, we’ve got our corners in place, and now it’s an opportunity to take each of those pieces of information and combine them to create that picture of you so that we really understand what we should be doing as we move forward. Now this is sometimes where I think it can get a little bit confusing for patients. Honestly, for even providers, this is that next level. That’s understanding not just an individual test but putting them together. When we combine them, what we’re really looking to do is create what is called a “risk assessment.” This means taking all of the different tests, putting them together, and then being able to give someone their risk status. A risk status tells us: is somebody in a very good place? We feel that they will do well long-term. They’re able to manage themselves and their activities without issues and concerns, or are patients struggling, and do we need to figure out what our next steps are going to be?
To try to give you a little bit better understanding of what all of that means, I think it’s always helpful to look at what an example of a risk assessment might be. Your provider may use this type of risk assessment, but there are others that can be used. I think most importantly is that we are combining all of the individual tests together to get a better understanding of you as a whole. Now when we look at this, we can see that we have a green zone, a yellow zone, and a red zone, and those are indicated by a low-risk status, an intermediate-risk status, or a high-risk status. And then within that, there are many different variables that we’re looking at. I’ll go through a few of them right now just to give you an idea of what we’re seeing when we’re putting these pieces together. The WHO-FC stands for Functional Class, and when we say a one or a two, again those were those indicators that our patient is doing well and able to participate in their life without any significant limitations, versus somebody who may be in a red zone where they’re feeling their symptoms just at rest.
The next one is that six-minute walk distance. That looks at how far our patients are able to walk. If they’re able to walk over 440 meters, that is an indication that their heart is feeling quite good, their lungs are working quite well, and that overall long term, they will likely do better, versus somebody who really can’t walk very far. The NT-proBNP, as we’ve talked about, is there, and we are able to measure. The level of that NT-proBNP or BNP is an indicator of whether someone’s heart’s under strain or not under strain. And as we take all of these different variables and tests, we’re able to score somebody so that we’re giving them their risk status.
So for this individual that, again, we’ve made up, but they’re feeling good, their Functional Class is in that green zone, their walk distance is above 440, but their NT-proBNP was a bit higher than we would want it to be. And when we looked at some of the tests from the right heart catheterization, they maybe weren’t in the range that we wanted, so they were in a yellow or intermediate-risk range there. As we move through all of these, we’re able to circle those different numbers or risk status and give a score, and at the end of it, that score indicates whether somebody is in their green zone, a yellow zone, or a red zone. That combination of tests and information then allows us to have a conversation with our patients in order to adjust a treatment plan if necessary.
Now, you may say, “That’s all fine and well, but what does it mean? Where are we trying to get? And if we get there, what does that mean for me?” The wonderful thing is that over the last 30-plus years, the amount of information and ability to affect someone’s care and health in PAH has grown. We now know that getting somebody into that low-risk zone is the goal for every patient, because it indicates that they will not only feel better, but they will live longer. So a low-risk status, as soon as we can get them there, is the goal—that’s the ideal. So we’re looking at preventing progression of PAH because we have them in a low-risk zone, their life expectancy over five years has improved, and they overall feel better and so can enjoy their life more.
So what can you do? Well, this is the piece that I always think is essential, because one, you’re already doing it because you’re here, and you’re learning, and you’re advocating for yourself to be able to then go forward in your journey or your loved one’s journey, and that really then comes back to those conversations with your specialists. I think it’s really important that you feel empowered to be able to have conversations and ask questions when you talk to your healthcare provider. You’re wanting to understand why maybe your test results have stopped improving, or you need to let them know that you’re experiencing new or worsening symptoms, and that maybe you don’t really know what your risk status is, or you have calculated it and realize you’re not at low risk. Those conversations are essential because those will help move the needle in your care. There’s a QR code that if you want to scan it, you can learn more about risk assessment and risk status in the corner of this slide.
Now, when we move on, we can also discuss the importance of finding the right specialist, and although there are many different people, and it’s sometimes difficult to navigate the healthcare system, not all cardiologists and pulmonologists necessarily specialize in PAH. And so there’s a QR code available, or you can visit FindAPAHDoctor.com, because that may help you navigate your area and find somebody that is right for you so that you can have those discussions since PAH is a rare disease.
All right, in summary: testing monitors your PAH status and how your treatment is working. Any changes in the heart and lungs may happen before you ever feel symptoms, and so it’s important to make sure that we are moving forward and testing appropriately to be able to catch that early. Test results are even more meaningful when we combine them together to form that risk status. Improving your risk status, hopefully to low risk, may be the key to feeling better and living longer.
It’s been my pleasure being with you today, and I look forward to our next PAH Today, where I will have an opportunity to explain the symptoms of PAH and hopefully give some insight into how you are feeling. So please join us next time at our second virtual event, which will be held on October 8th, 2022, at 2 PM to 3 PM Eastern Standard Time. Register today at www.PAHtoday.net. Also consider joining the PAH Initiative at PAHinitiative.com, where you can stay informed, stay motivated, stay focused on your future. Thank you, and again, we appreciate you being here. I appreciate you being here. Continue to advocate for yourself, and if you want more information, please visit www.PAHinitiative.com.
What do your tests results say about your PAH?
Explore how your combined test results give you and your specialist the big picture of your unique PAH.
PAH Life Expectancy & Risk Status