What are the symptoms of PAH?
You may notice symptoms but not realize they may be a sign of pulmonary arterial hypertension (PAH). This is because PAH may affect people in different ways, and as a result, symptoms can look quite different from one person to another.
As the blood vessels in your lungs thicken and narrow due to PAH, higher pressure in those vessels reduces blood flow within the lungs. Over time, the heart becomes strained as it works harder to push blood through the narrowed vessels.
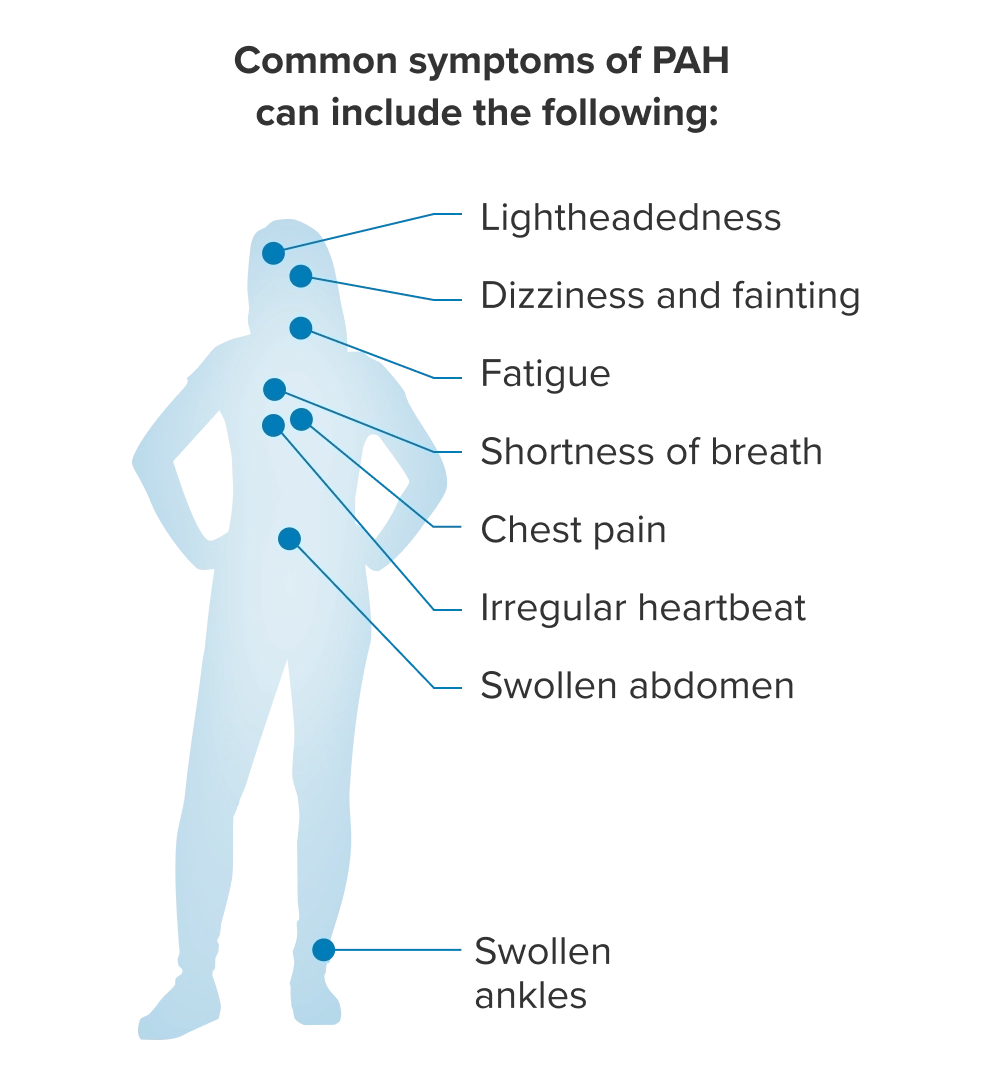
Fatigue, lightheadedness, and an irregular heartbeat can occur as a strained and less efficient heart works harder to keep up.
Dizziness and fainting can occur as the heart strain becomes more severe. As the strain on the heart gets worse over time, eventually, the heart can begin to fail.
Shortness of breath and chest pain can occur due to the body not getting enough oxygen, because of reduced blood flow through the lungs.
Swelling in the abdomen can occur when blood backs up in the liver and kidneys.
Swollen ankles can be a sign of increased fluid or water retention caused by high blood pressure and/or excess sodium.
Symptom checklist
Download the checklist to make the connection and guide a more helpful talk with your doctor about treatment planning.
Download Symptom ChecklistKnowing your symptoms matters
Dr. Lana Melendres-Groves shares important advice: Don’t wait to talk to your doctor about PAH symptoms like shortness of breath and chest pain. The sooner you start or change treatment, the better you may feel.
Knowing about the symptoms you experience and when you experience them helps your healthcare provider assess whether your condition is improving, staying the same, or getting worse. This is key to determining the right treatment plan. You are likely familiar with at least some of the PAH symptoms like shortness of breath, a rapid, hard, irregular heartbeat, chest pain, swollen ankles, a swollen abdomen, or even dizziness and fainting. Over time, as the disease progresses, the symptoms get worse and you may find that you cannot do as much physically. It’s important to note that symptoms may not always reflect whether PAH is progressing or how it is affecting your body. Even if your symptoms remain the same, there still may be more you can do to help improve how you feel. Sometimes people with PAH try to ignore their symptoms until they become more extreme, but when it comes to PAH, it’s important to speak with your doctor about how you are doing.
Effectively treating PAH sooner rather than later can make a difference in how quickly your PAH progresses. So it’s important to be your own advocate and to find an experienced PAH doctor. Not all pulmonologists and cardiologists have specialized PAH training, so it’s important to find a PAH doctor who understands each of the available PAH medications.
Reducing your PAH symptoms is an important goal
Improving PAH symptoms is a common goal for patients and their healthcare teams. Fortunately, medications can help widen the blood vessels in your lungs. They can also slow down the narrowing of the vessel passages that put strain on your heart as it struggles to keep up.
Taking a closer look at your symptoms
As PAH progresses, you may find that performing routine activities becomes more and more difficult. You may feel worn out, and you may even faint.
It is important to monitor and track your symptoms closely and promptly communicate any changes to your healthcare provider
PAH symptoms may be a sign it’s time to try something else
If you are still having symptoms, your current treatment plan may not be doing enough to control the progression of your disease. If you’ve stopped improving and aren’t where you want to be, talk to your healthcare provider about additional options.
You can learn more about what’s going on in your body that causes PAH symptoms at the link below.
What Is PAH?What can you do to improve your symptoms?
You play an active role in your care! When you monitor your symptoms and tell your PAH specialist about any changes, it helps them figure out the best way to treat you. They can also decide if any changes need to be made to your treatment plan. Some changes they might talk to you about could be eating healthier, exercising more, or trying a new medication.
Improving your symptoms may not only help you feel better now so you can continue to do the activities that you enjoy, but it can also help improve your prognosis and the future course of your PAH.

“You need to be honest with your doctor, let them know what you want to do. And you and him, come up with the best plan that you both can handle.” —Gwen, PAH Initiative Ambassador

Improving your symptoms could have a positive effect on your future
Improved symptoms could also improve your risk assessment, increasing the chances you’ll be doing better in the future. So, what is risk assessment? It’s a comprehensive assessment that combines your individual test results to give a holistic view of your PAH.
Why having a PAH specialist matters
Not all healthcare providers have experience treating PAH. Healthcare providers with experience treating many PAH patients have specialized training and know how to evaluate changes to your PAH symptoms and make adjustments to your treatment plan so you can keep improving.
Patients with PAH should see healthcare providers who are specialists in PAH.
Find a PAH Specialist
Discuss your symptoms with a PAH specialist
Prepare to discuss your symptoms, treatment goals, and care plan with your specialist—download this discussion guide to get the conversation started.
Download Doctor Discussion GuideGet the guide via email
Get the guide sent to you so you can review it later.
Get the guide sent to you so you can review it later.
Create an event reminder
Set a reminder for your next appointment that includes the guide (and your notes) in the description.
Set a reminder for your next appointment that includes the guide (and your notes) in the description.
Understanding your PAH symptoms
Get answers to your key questions from a PAH expert. Dr. Vijay Balasubramanian explains the relationship between pulmonary pressure and symptoms—and what active steps you and your specialist can take (including treatment changes) to help improve your symptoms.
Hello, everyone. I'm Dr. Vijay Balasubramanian. I'm one of the pulmonologists, the medical director for Valley Advanced Lung Diseases Institute here in Fresno, California. I'm also a specialist in pulmonary hypertension and advanced lung disease. It's great to meet all of you, and here today we are going to talk about understanding your pulmonary arterial hypertension symptoms.
This presentation is sponsored and made on behalf of United Therapeutics. Speakers are compensated by UT. The information presented here is for educational purposes only and is not intended as professional medical advice. Always discuss questions you may have with your healthcare provider. Not all medications are appropriate for all patients. Please speak with your healthcare professional to determine which treatment plan is right for you.
Today's overview of the presentation is basically in three steps. Pulmonary arterial hypertension, how does it affect your body? And PAH medications, how do they improve symptoms? And what can you do to help in this process?
How does pulmonary arterial hypertension affect your body? Pulmonary arterial hypertension is a rare and a serious lung disease. The blood vessels within the lungs tend to thicken and narrow over a period of time. This makes it hard for the right side of the heart to squeeze the blood into the lungs, and therefore, it has to generate higher pressure in the blood vessels, and therefore, lesser blood flow within the lungs.
The narrowed vessels and less blood flow affects different parts of your body. Obviously the more common symptoms being shortness of breath and fatigue. And eventually, as the right side of the heart starts becoming more enlarged and strains and becomes weaker, then what we call the failing right side of the heart, then the swelling in the abdomen happens. Swelling in the ankles can happen due to more fluid and water retention as a result of this high pressure that's generated in the lung circulation. And shortness of breath and chest pain may occur due to the body not getting enough oxygen.
The blood vessels in your lungs are like highways. Here is a nice cartoon that illustrates how the blood travels within the blood vessels. When the highways work best with fully open lanes, you can see all the cars are running smoothly in their respective lanes. But when you see that there is a lane closure, you can see things backing up and the pressure builds up. And that's typically what happens within the blood vessels of the lungs. The narrowed blood vessels cause more resistance, and that is what we call or refer to as pulmonary arterial hypertension, which leads to less blood flow, and therefore, less oxygen transfer. The higher resistance in the lungs causes higher pressures in the heart, and the right side of the heart swells, enlarges, and therefore, it makes it harder for the right side of the heart to push blood through these narrow vessels. The less blood flow through the lungs lead to less oxygen reaching the parts of your body where it's needed. So adequate blood flow and oxygen are important factors for normal bodily functions to carry out day-to-day activities. That is how a patient might end up feeling short of breath or fatigued when even doing daily tasks.
The heart becomes strained over time. To compensate the strained heart pumps more forcefully trying to push blood through these narrowed vessels and this can result in fatigue, lightheadedness. And the type of lightheadedness we see in pulmonary arterial hypertension is when patients engage in activity, meaning to say, the more oxygen a patient needs, that is when the strain is felt more and they feel more lightheaded because the body is just not able to compensate for the increased need.
The strain on the heart can get worse over time, and this can lead to what we call heart failure. As the heart enlarges and strains, it won't be able to keep up and will begin to fail at some point. Patients can start feeling dizzy and can even faint with even some exertion.
Now, that is why diagnosis of pulmonary arterial hypertension can really help because once we make the diagnosis and get the patients on appropriate PAH medications that can improve the blood flow in the lungs and that reduces the strain on the heart.
How do PAH medications help improve symptoms? Healthy blood vessels require a balancing act. Basically, you have certain chemicals that help to keep the blood vessels open, and there are certain chemicals that keep the tone of the blood vessels, meaning to say it has to remain in a good tone. A healthy balance between the two helps for adequate blood flow through the blood vessels. But when you have certain substances, when this balance gets tilted one way, there might be too much of some substances and too little of others. Then you might see progressive narrowing of the blood vessels, and therefore, increases the blood pressure in the lung circulation.
Most people have more than one substance out of balance. PAH medications can help restore that balance, so can slow down the production of substances that you have too much of or increase the production of substances that you don't have enough of. Please talk to your doctor about your treatment plan if you have stopped improving or still experiencing PAH symptoms despite some treatment changes because this is a dynamic thing. It'll constantly keep moving, depending on each and every patient, depending on their status.
PAH medications can help traffic flow more smoothly. They can help widen the blood vessels in the lungs or open more lanes, so to speak. Now, they can flow more effectively and it reduces the pressure in the process. The resistance to flow gets lower and the blood begins to flow more normally. The treatment guidelines recommend treatment with two or more types of PAH medications for most patients. Again, just as we spoke about a couple of slides ago, most of the time, patients can have more than one chemical imbalance, and therefore, targeting at least two mechanisms can help improve outcomes. And what do we mean by outcomes? The improved functional class improved ability to do more activity and feel less short of breath, and that is what is measured in the six-minute walk distance as well. These type of improvements can be achieved with the help of this type of approach. So taking a combination of medications may improve how well you can do your day-to-day activities with minimal or less symptoms.
The right combination is the one that helps you meet your treatment goals, and the treatment goal is something that you have to set along with your provider. And what do we mean by that? What we mean by a treatment goal is improving lung function, improving heart function, and improving symptoms. The treatment goals are very much set by yourself in partnership with your provider, so you and your healthcare provider will choose the type of medications that can best treat your unique PAH.
What can you do? Take an active role by tracking your symptoms. Please be observant. Keep track of your symptoms in a way that works for you, such as a symptom journal is just an example, including activities that you can do without symptoms, activities that trigger symptoms. That way, when your healthcare provider asks you the next time, "What are the challenges that you're experiencing?" you can be very succinct in telling what your challenges are. Please share your symptoms with your healthcare provider at each visit. And the dynamic nature of improvement or worsening can be assessed by yourself in this process.
Not all cardiologists or pulmonologists have expertise in treating PAH. It's important to find a provider with specialized training in pulmonary arterial hypertension, who has experience in using all classes of PAH medications. PAH treatment guidelines recommend working with a PAH specialist. To help you find a list of PAH specialists, you can refer to the Pulmonary Hypertension Association website or you can scan the QR code. Visit findapahdoctor.com. That might give you that information.
Discuss your options with a PAH specialist such as adjusting your medication plan, adding or changing your medication, adjusting the dose of your medication. Please start making lifestyle changes, like starting an exercise program, changing your diet such as limiting salt intake, and getting rest and emotional support is very important as well. There may be more you can do to help reduce your PAH symptoms and do more daily activities.
In summary, in PAH naturally occurring substances in your lung blood vessels, can become imbalanced. The imbalances in the blood vessels prevent your lungs and heart from working properly. Treatment with a combination of medications may help restore this balance and improve PAH symptoms. Talk to your doctor about your treatment plan. They may be able to do more for you, and obviously you yourself have a great part in this.
Thank you. I hope this information was very helpful. Consider joining the PAH initiative at jointhepahinitiative.com, and you can also follow us on social media. Thank you.
What types of treatments are available for PAH?
Learn more about the kinds of PAH medications available and how they may help improve PAH symptoms.
PAH Treatment Options
