Find the knowledge you need to help you manage your path forward with pulmonary arterial hypertension (PAH). Access videos, infographics, guides, and brochures that provide trusted information on how PAH affects your heart and lungs, treatment approaches and goals, and actionable tips for daily living.
For more educational materials in Spanish, visit our Spanish-Language Learning Library page.
Para más materiales educativos en español, visite nuestra página de Biblioteca de Aprendizaje.
Hi, I’m Dr Lana Melendres-Groves, a pulmonary arterial hypertension specialist and director of the Pulmonary Hypertension Program at the University of New Mexico. I have been treating pulmonary diseases for over 12 years with a specialization in PAH for over 9 years. My clinic has treated over 5,000 patients, and I currently oversee 250 PAH patients on PAH-specific medicines. In this video, we’ll cover the basics of pulmonary arterial hypertension, also known as PAH. Understanding what PAH is can be confusing because even healthcare providers may tell you different things about it. Some may say your heart doesn’t work as well as it needs to. It’s really about the blood vessels. The real problem is in the lungs or it’s just hypertension. This is why it’s so important to find an experienced PAH specialist to help you. A PAH specialist is a cardiologist or pulmonologist who has had specific training in PAH and understands how challenging this disease really is.
The heart, lungs, and blood vessels all work together as a cardiovascular team and PAH affects each of these vital organs. So, let’s start with the heart. You may already know that the heart has 4 chambers. Two chambers are called “atria” and receive blood from the other parts of the body, and the other 2 chambers are called “ventricles” and pump blood out of the heart. The right atrium receives blue, oxygen-poor blood from the body and the right ventricle pumps that oxygen-poor blood to the lungs where it can pick up oxygen. The left atrium receives red, oxygen-rich blood from the lungs and then the left ventricle pumps the oxygen-rich blood to the rest of the body. Although cardiac diseases, including heart attacks, are more common in the left ventricle, it’s actually the right ventricle that is affected in people who have PAH.
Again, the heart, lungs, and blood vessels all work together. PAH begins when the walls of the blood vessels in the lungs thicken and become more narrow. Because the blood vessels become more narrow, it’s harder for the blood to pass through them. The reduced blood flow that is caused by the narrowed vessels creates increased pressure on the right side of the heart. The right side of the heart tries to compensate by working harder to pump blood through the vessels and into the lungs. Over time, the heart struggles to maintain this level of intensity. It’s like asking your heart to run a marathon every minute of every day and PAH symptoms result. Because sending blood to the lungs is somewhat easier than pumping blood to the entire body, the right ventricle was not designed to work quite as hard as the left, but working so hard to compensate for narrowed blood vessels causes the right side of the heart to enlarge and eventually to weaken so that it wears out and is no longer able to keep up. One analogy that can help with understanding PAH is traffic on a 5-lane highway.
The highway represents the blood vessels and the cars represent the blood cells. Watch what happens to the traffic flow when there is construction. If 2 lanes on the 5-lane highway are closed for construction, it’s harder for the cars to get through. Traffic flow slows down and the cars back up behind the lane closure, causing a traffic jam. In your body, narrowed blood vessels cause the blood flow to slow and back up into the right side of the heart as it struggles to keep up. This means less blood is able to get pushed through the lungs to pick up oxygen. Because the heart has to work harder to pump blood into the lungs, people with PAH begin to experience symptoms such as chest pain and shortness of breath. Although symptoms help doctors diagnose PAH. They are also a critical element of monitoring PAH over time.
Knowing about the symptoms you experience and when you experience them helps your healthcare provider assess whether your condition is improving, staying the same, or getting worse. This is key to determining the right treatment plan. You are likely familiar with at least some of the PAH symptoms like shortness of breath, a rapid, hard, irregular heartbeat, chest pain, swollen ankles, a swollen abdomen, or even dizziness and fainting. Over time, as the disease progresses, the symptoms get worse, and you may find that you cannot do as much physically. It’s important to note that symptoms may not always reflect whether PAH is progressing or how it is affecting your body. Even if your symptoms remain the same, there still may be more you can do to help improve how you feel. Sometimes people with PAH try to ignore their symptoms until they become more extreme, but when it comes to PAH, it’s important to speak with your doctor about how you are doing.
Effectively treating PAH sooner rather than later can make a difference in how quickly your PAH progresses. So, it’s important to be your own advocate and to find an experienced PAH doctor. Not all pulmonologists and cardiologists have specialized PAH training, so it’s important to find a PAH doctor who understands each of the available PAH medications.
Things to remember: PAH is a disease of high blood pressure within the blood vessels of the lungs that leads to right heart damage and eventually heart failure. The symptoms that you feel are a reflection of how your heart is struggling and they will not improve without treatment. PAH is a progressive disease, meaning that it will get worse over time, but the rate of progression varies. Be proactive by finding a doctor who specializes in PAH and ask about things you may be able to do now to reduce symptoms and help slow disease progression. I’ll leave you with this tip: Keep a symptom journal. Either on paper, on your computer, on a mobile device. That way you won’t have to try and remember everything that happens between doctor visits. This will help you and your healthcare provider determine whether your PAH symptoms are changing over time and what treatment options may be best for you.
Thank you for watching PAH Basics. Watch the next video from the PAH Initiative video series to learn about working with your PAH doctor to set goals for treatment.
[End of video: PAH Initiative, Sponsored by United Therapeutics, Committed to Improving the Lives of Patients. For more resources about PAH, please visit www.PAHInitiative.com. Copyright 2019 United Therapeutics Corporation. All rights reserved.]
Welcome back to the PAH Initiative video series. I’m Dr. Lana Melendres-Groves, a pulmonary arterial hypertension specialist and director of the Pulmonary Hypertension Program at the University of New Mexico. I have been treating pulmonary diseases for over 12 years, with a specialization in PAH for over 9 years. My clinic has treated over 5,000 patients, and I currently oversee 250 PAH patients on PAH-specific medicines. In this video, we’ll discuss the goals of treatment and plans to address those goals. If you haven’t seen the PAH Basics video, it’s better to watch that first. Goals are important to help us assess whether treatment is working well enough or if there’s need to make treatment changes. My PAH patients usually have their own personal goals in mind, and as a pulmonary arterial hypertension specialist, I have clinical goals for my patients as well. Fortunately, these goals work hand in hand because achieving clinical goals may help patients achieve their personal goals as well. Although the words are different, the important thing is that you and your doctor discuss your treatment goals and make sure you understand each other.
Personal goals for patients with PAH often include experiencing fewer symptoms such as fatigue and shortness of breath, spending less time in the hospital or not being hospitalized at all, being more active, or even spending more time with friends and family, and getting out more. Physician PAH treatment goals include improving right ventricular heart function, having healthier blood vessels in the lungs, and slowing disease progression. Let’s talk about how you and your doctor can work together to reach these goals. I want to start by familiarizing you with the phrase, risk status, which you might not have heard of before. Risk status is a different way of looking at your PAH. It involves some of the tests that your doctor’s already using to monitor your status. But it goes beyond just looking at how you’re doing today. A risk assessment uses the results to predict how your PAH may change over the next 5 years. PAH specialists now consider improving your risk status as an important treatment goal.
Risk status is either low risk, intermediate risk, or high risk. Low risk means that there’s a low chance of your PAH getting worse. If your level is intermediate or high risk, there’s a higher chance that your disease will get worse. When PAH disease gets worse, it’s referred to as disease progression. If your status is high or intermediate risk, your doctor may want to consider changes in your care by adjusting your treatment plan to help improve your risk status and lower the chance of your disease getting worse. Your doctor will look at a number of different factors to evaluate your risk status. Three commonly used assessments are the 6-minute walk test, NT-proBNP and BNP, which are blood tests, and Functional Class.
Let’s consider each of these assessments a little more closely. You may already be familiar with the 6-minute walk test. It is a test to see how far you can walk in 6 minutes. Performing a 6-minute walk test at each doctor’s visit provides an important view of your status over time. This helps your doctor assess whether your treatment might need adjustment. You might be interested to know that the average walking distance for patients with PAH in 6 minutes is approximately 350 meters. Patients considered low risk can walk more than 440 meters in the walk test. And the average distance for people who do not have PAH is between 590 and 640 meters.
Did you know that a meter is slightly longer than a yard? In other words, a 100-yard football field is a little over 91 meters long, so 440 meters is equal to a little less than 5 football fields. Being able to walk further during your test indicates that your heart, lungs, and blood vessels are functioning better than when you did not walk as far. Improving walk distances over time is a goal PAH doctors set for many of their patients. This is one part of the larger goal of trying to improve risk status.
Another test that’s considered in risk assessment is a blood test called “NT-proBNP” or “BNP.” BNP is a chemical the heart makes when it is strained, NT-proBNP is another form of this chemical. So it makes sense that there’s more BNP if the heart is under greater strain. Although no one test determines your risk status, an NT-proBNP greater than 300 nanograms per liter, and BNP greater than 15 nanograms per liter indicates that the heart may be working too hard.
Functional Class is another type of evaluation that can be used to help assess risk status and is an indicator of your capacity to physically function. How much activity you are able to do without experiencing symptoms determines your Functional Class. Class 1 means you have no symptoms with ordinary physical activity. Class 2 means you have symptoms that slightly limit your activity. Class 3 means that your symptoms significantly limit your activity. And if you have symptoms even while resting, that is considered a class 4. Functional Class 1 and 2 are associated with low-risk status. What I tell most of my patients who are high risk or intermediate risk, is that we should strive for low-risk status. In 3 to 6 months, we’ll see if we’ve gotten there, and if not, we will consider what else we can do to help them try to achieve their goal. Talking to your physician about your risk status is a starting point for setting goals and creating a treatment plan.
Once again, healthcare providers assess risk status using 6-minute walk test, BNP blood tests, and Functional Class, as well as other tests. Changes in your test results can show how your treatment is working and if your treatment needs to be adjusted. I’ll leave you with this tip, be proactive by making a list of your treatment goals to see if they match your healthcare provider’s goals. Ask your provider if lowering your risk status is one of your treatment goals and what more you can do to meet your goals. Thank you for watching PAH treatment goals. Watch the next video in the PAH Initiative video series to learn about working with your healthcare provider to learn about treatment options available today.
Imagine you’re driving your car and it becomes imbalanced and wobbly. Why? Because several of your tires have either too much or too little air pressure. Now your car isn’t functioning as it should, and your ride has become quite bumpy. What would you do? Would fixing only one or two of the tires be the best solution if more of the tires are affected?
Of course not.
So, we know a car will run more smoothly with balanced tires. In a similar way, your body needs the right amount of each of 4 natural substances to keep your lungs and blood vessels healthy. Normally, the body produces the right amount of these substances, but in people with pulmonary arterial hypertension, or PAH, an imbalance in 1 or more of the substances can affect blood vessels, causing the walls to thicken and narrow. This results in PAH symptoms and strain on the heart over time as it struggles to push blood through the lungs. This is where PAH medications come in.
Just like a mechanic adjusts the tires to restore your car for a smoother ride, medications may help balance the substances in your body to keep the blood vessels in your lungs healthy.
Now, knowing which substances are imbalanced and the extent of each imbalance isn’t as easy as fixing a tire. In PAH, there’s no test to pinpoint imbalances, like how a tire gauge shows when tires need air. It’s as if we can’t see the tires, but we can tell something is wrong because of the bumpy ride. Based on clinical trials, we do know that most people with PAH have at least 2 substances out of balance. That’s why experts recommend most patients take two or more medications to address these imbalances. Understanding the role of these substances in PAH and the need to rebalance them can empower you to have informed treatment discussions with your healthcare team. And just like driving a well-maintained car, navigating life with PAH may become smoother with the right balance and care.
So, if your ride is still bumpier than you’d like, ask your PAH specialist if you can do more to get closer to balance.
I’m Dr. Lana Melendres-Groves, and I’m the Medical Director for the Pulmonary Hypertension Program at the University of New Mexico. Today, I want to start by asking you a simple yet meaningful question.
How are you really feeling?
If you’re living with PAH, taking a moment to ask yourself this question regularly is important. Healthcare providers often see patients who do not prioritize themselves and their health as much as they should. For example, people with PAH may not speak up when they’re not feeling well, potentially missing the opportunity to discuss changes to their treatment plan that could help them feel more like themselves again.
Knowing this, let’s revisit those substance imbalances that contribute to your PAH symptoms and explore how each imbalance can be addressed by a different PAH medication.
We’ve learned that people with PAH typically have an imbalance in 2 or more of the natural substances that play important roles in keeping the lungs’ blood vessels healthy.
Each substance imbalance corresponds with what PAH experts call a treatment pathway. The 4 PAH treatment pathways are the nitric oxide, endothelin, prostacyclin, and activin signaling pathways. And the good news is that each pathway has a type of medication that can help rebalance it. To understand this better, let’s take a closer look at the 4 pathways that medications treat.
First, let’s talk about the nitric oxide pathway. People living with PAH may not produce enough nitric oxide. Medications that treat the nitric oxide pathway help replace the nitric oxide that may be missing in PAH. These medications are available in pill form for patients who have been recently diagnosed with PAH. Medications for this pathway help open the blood vessels in your lungs, allowing blood to flow more easily and reducing pressure on your heart.
Now, let’s look at the endothelin pathway. People with PAH may produce too much endothelin. So, medications targeting the endothelin pathway help reduce the extra endothelin your body produces. In turn, these medications help open blood vessels and slow down the thickening of the vessel walls. Medications that treat the endothelin pathway are available in pill form and are often prescribed for patients who have been recently diagnosed with PAH.
Let’s move on to look at the prostacyclin pathway now. It’s another important one. People with PAH may not produce enough prostacyclin. Medications that treat the prostacyclin pathway help replace the missing prostacyclin. This may also help open blood vessels, slow down vessel wall thickening, and prevent clotting. Finding the right dose of a prostacyclin-class medication can help ensure it’s providing the most benefit. Medications that treat the prostacyclin pathway come in three different forms: inhaled, pill, and infused. Many patients prefer the inhaled form, as it delivers the medication directly to the lungs. Prostacyclin-class medications are recommended by PAH experts for patients at high-risk status upon diagnosis or to be added to treatment plans for patients who aren’t getting to low-risk status quickly enough.
The fourth and final pathway is the activin signaling pathway. The medication targeting this pathway helps address a complex substance imbalance. Doing so may help control overgrowth in blood vessels. This medication is available in injection form and is typically added to a treatment plan for patients who are not getting to low-risk status quickly enough. This medication is often used in combination with other medications, including prostacyclin-class medications.
So, we have four different pathways, with medications to treat each. But how do we know when it’s time to switch, combine, add, or change the dose of medications? PAH experts believe risk status helps you and your doctor know how well your treatment is working. Risk status combines your test results, your symptoms, and other important clues into an overall picture of your unique PAH. This helps tell you if you are on the right track or if it’s time to make an adjustment.
For most patients, one important goal is achieving low-risk status. When patients are at low-risk status, they are likely to feel better and walk farther with fewer symptoms. Regular risk assessments by your PAH specialist can help ensure you are headed in the right direction. This is why you need to have frequent communication with your PAH specialist. Be sure to keep on top of regular appointments, and also keep your specialist informed of exactly how you are feeling. What you tell your specialist helps personalize your treatment plan.
So, we’ve talked a little about how we determine when it may be time to add or change PAH medications. But how do we know which of the available medications to use? Well, while no single test can pinpoint the exact imbalance you may have, years of PAH patient research, as well as listening to your symptoms, provide important clues.
We know which medications are typically prescribed first and which are added later if risk status isn’t showing adequate improvement. Adding a medication can help many patients get the most out of each day. Another consideration is adjusting the dosage of medications to get the best possible results from your treatment plan.
Understandably, many of my patients are sometimes reluctant to add another medication. But feeling unwell isn’t ideal, either. Ultimately, the key is to really consider the potential benefits and work closely with your specialist to navigate any challenges and side effects. If you are already on PAH medications but not tracking toward your goals or feeling as well as you’d hoped, then consider asking your specialist about adding another medication. It’s more than okay to ask questions and explore your options. It’s crucial. Your PAH specialist is there to listen, is equipped to answer questions, and can help you make informed decisions. Adding a PAH medication or modifying your treatment plan may help improve PAH symptoms, allowing you to do more activities and feel more like yourself.
In between ‘doctors’ visits, you can visit the PAH Initiative. There, you can learn more about PAH and find a guide to help you talk to your specialist. If you don’t have a PAH specialist, the website can also point you toward finding one.
Earlier, I asked you how you were really feeling. Have you thought about it recently? If you are not feeling as well as you’d like, now is the time to take action. Ask your specialist if adjusting your treatment plan could be the right next step.
We can’t always see what’s over the horizon. That doesn’t mean we don’t have options for getting there. Keep going. Prioritize you. And remember, you are not alone.

Use this discussion guide to plan the things you’d like to discuss with your healthcare team. It addresses topics like your symptoms, test results, and treatment options.

Learn what to expect from a right heart catheterization, with clear answers to common questions and a useful appointment checklist to help you prepare.

Explore how PAH impacts your body, risk status, different ways to treat PAH, how to prepare for conversations with your doctor, and more.
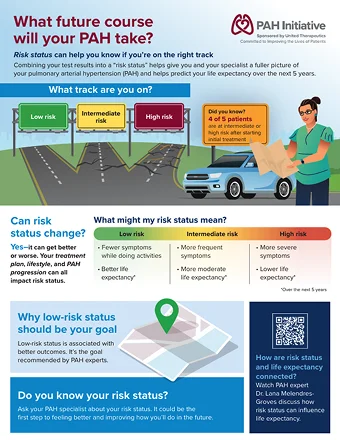
Learn all about risk assessment: how and why it works, its importance, and its role in guiding PAH care.
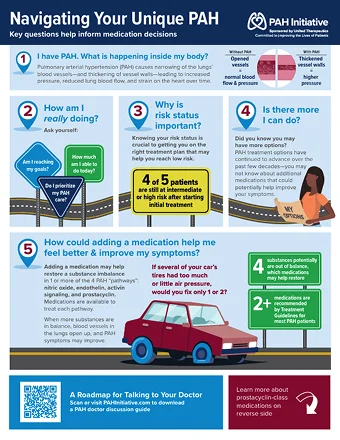
Get a big-picture perspective of PAH as you explore how it affects your heart and lungs and how specific medications target “PAH pathways” to help you feel better.

Some of the ways to relieve stress are obvious, like yoga. But music, gardening, laughter—and even chewing gum—can help you relax and ease your stress.

This 1-page guide provides websites full of recipes and tips that can help you cut back on salt. You’ll also learn to understand nutrition labels and find suggestions for those times when you’re dining at a restaurant or with friends.

Get more flavor in your diet with nutritious smoothies. These 8 smoothie recipes offer flavors like peanut butter banana, cherry chocolate, and key lime pie.
Sign up to receive updates from United Therapeutics and the PAH Initiative.
Sign Up