PAH: A rare and progressive disease
Group 1 pulmonary arterial hypertension (PAH) is a rare subset of pulmonary hypertension.1 PAH is a serious, progressive disease of the lungs, primarily affecting small pulmonary arterioles.2 Over time, the pathophysiology of PAH causes progressive blood flow restriction and right heart ventricular dysfunction, eventually leading to heart failure and death.2,3
PAH is WHO Group 1
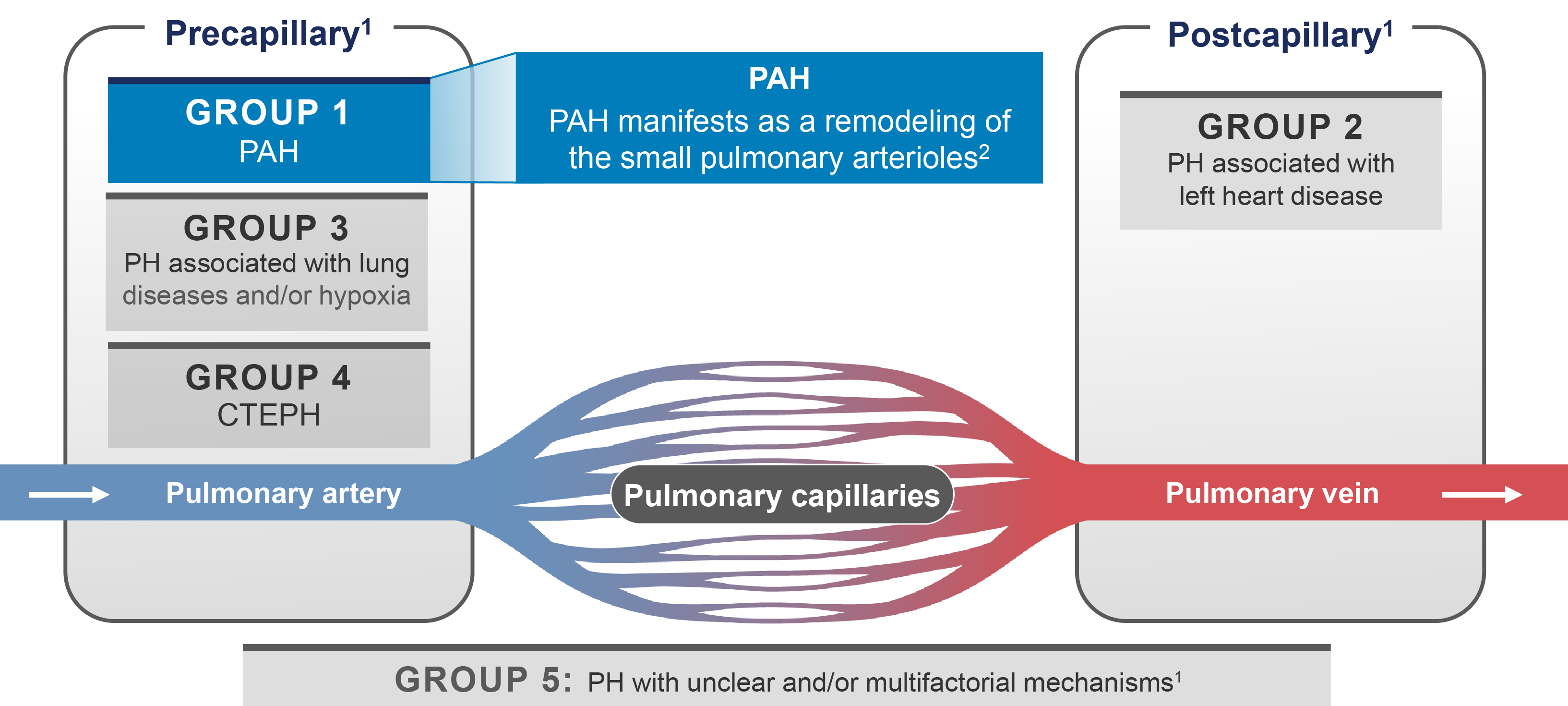
PH is categorized into 5 groups based on pathophysiology, clinical features, and therapeutic approaches1:
-
Group 1
PAH: Precapillary PH characterized by increased pulmonary vascular resistance in the absence of other causes of precapillary PH (ie, lung diseases or thromboembolic events)
-
Group 2
PH due to left heart disease: Includes patients with PH caused by left heart conditions (ie, left ventricular dysfunction or valvular disease), where elevated left heart pressures lead to increased pulmonary pressures
-
Group 3
PH due to lung diseases and/or hypoxia: Includes patients with PH who have chronic lung diseases (eg, ILD or COPD) or low oxygen levels, leading to high pulmonary pressure
-
Group 4
CTEPH: Patients with PH caused by chronic blood clots in the lungs, often treated surgically
-
Group 5
PH with unclear and/or multifactorial mechanisms: Encompasses PH cases with complex or unknown causes, including blood, systemic, or metabolic disorders
The cause of PAH is often unknown3
PAH falls into 6 general clinical classifications based on etiology:
Classification1
Details1,4
Idiopathic
Cause is unknown
- Includes PAH long-term responders to CCBs
Heritable
BMPR2 is the most commonly mutated gene
Drug- and toxin-induced
May include:
- Aminorex
- Benfluorex
- Dasatinib
- Dexfenfluramine
- Fenfluramine
- Methamphetamines
- Toxic rapeseed oil
Associated
May include:
- CTD
- HIV infection
- Portal hypertension
- CHD
- Schistosomiasis
PVOD/PCH involvement
Persistent PH of the newborn
For most patients, PAH has an unknown etiology or is associated with another condition5

The breakdown of PAH by etiology is:
- Associated PAH: 51%
- Idiopathic PAH: 44%
- Heritable: 4%
- Other: 1%
The most common associated condition is CTD, followed by CHD5

The prevalence of associated conditions is:
- CTD: 67%
- Portal hypertension: 9%
- Drugs/Toxins: 9%
- HIV: 4%
- CHD: 12%
- Other: 1%
PAH prevalence and patient characteristics

~1000 new cases are diagnosed in the United States every year8

PAH is more commonly diagnosed in women (70%-80% of cases)3

~2 years from symptom onset to diagnostic catheterization5

Average age: 50 years9*

61% 5-year survival average10

"Early recognition is really important and it’s important to collaborate … to recognize this patient population because they’re not all in highly dense areas. The earlier we recognize pulmonary hypertension, the earlier we can treat pulmonary hypertension, and the better the patients do."
— Dan Lachant, DO, Assistant Professor of Medicine, Strong Memorial Hospital/University of Rochester, Rochester, NY
